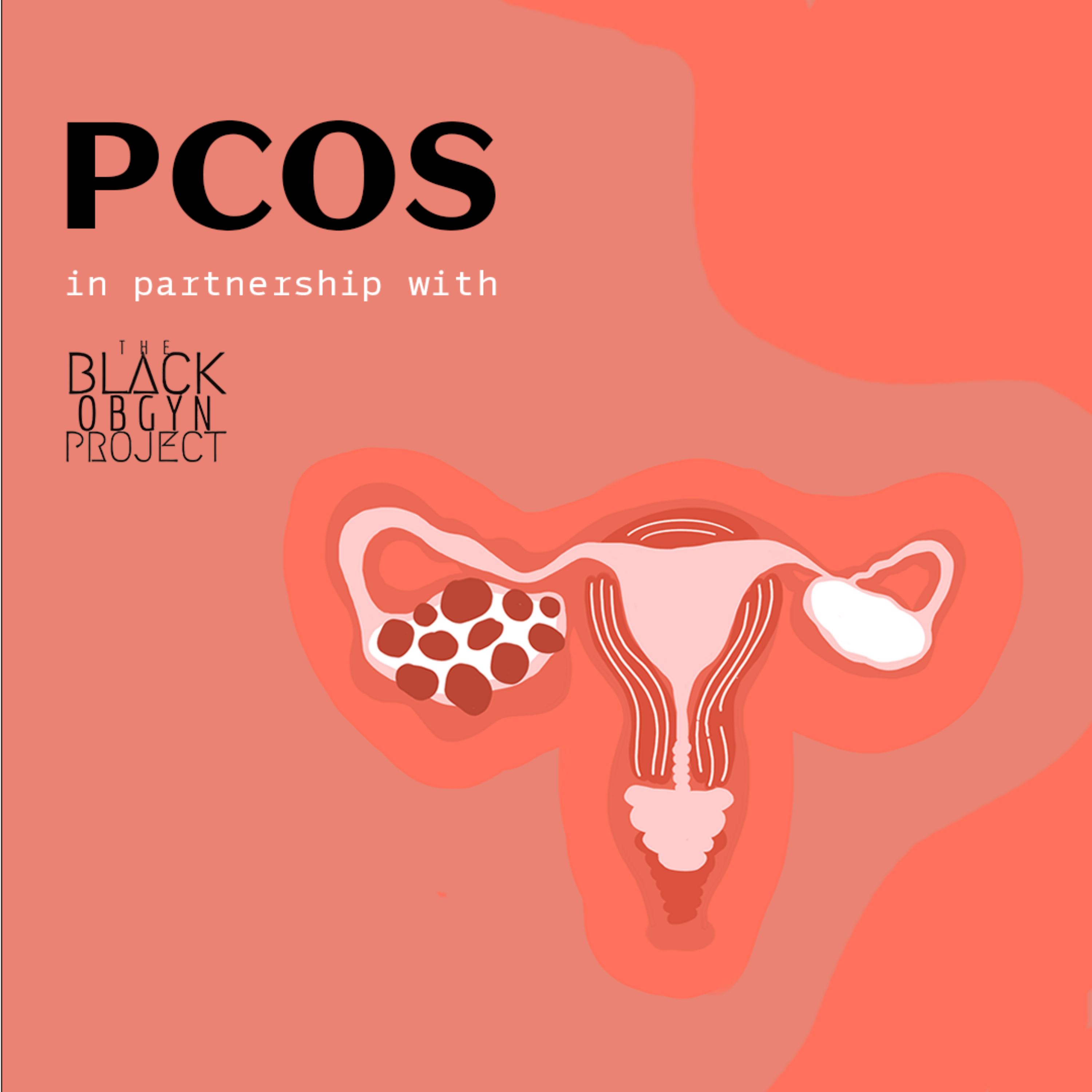
There’s a lot of acronyms every young women should remember, laugh out loud (LOL), Oh my God (OMG), You only live once (YOLO) and my personal favorite On my way (OMW), frequently used when I know full well that I haven’t even hopped in the shower yet. But, have you ever heard of PCOS? If not, this is definitely one you’ve got to add to your list. It’s an acronym for the most common hormonal abnormality among reproductive aged women and it stands for polycystic ovarian syndrome (PCOS). It’s a mouthful, which is fitting for a disorder that can cause a whole lot of problems.
So what is this cystic business and what does it have to do with ovaries? Well buckle up and hang tight because we’re about to take a deep dive into the world of PCOS. This particular syndrome affects 7% of women of child bearing age. PCOS is a hormonal disorder that creates somewhat of a snowball effect, increasing a woman's risk factors for multiple disease processes if left untreated. The most common criteria for diagnosis of PCOS is known as the Rotterdam criteria. It details three different clinical symptoms and a patient must have two of the three symptoms to be diagnosed with PCOS. These include, hyperandrogenism, a fancy word for high levels of male hormone, irregularities in menses, and polycystic ovaries. Now, before you start to self diagnose let’s talk about what these clinical symptoms really look like in the typical person. It’s not always easy to spot someone with hyperandrogenism. Some women can present with hirsutism, or male pattern hair growth, including around the chin and upper lip. Others can present with severe acne and still others can present with male pattern hair loss or alopecia. These symptoms can range from mild to severe. Using the Rotterdam criteria hyperandrogenism is diagnosed with either hirsutism or a blood test demonstrating high androgen, or male hormone levels. Menstrual irregularities is the second of the three criteria. Many women can have menstrual irregularities for a variety of reasons, pregnancy being the most common cause. In PCOS, women have oligomenorrhea which are menstrual cycle lengths (time between periods) that are greater than 35 days. Women with PCOS can also have amenorrhea which is a complete lack of menstruation. The third criteria for diagnosis of PCOS are polycystic ovaries. There are no symptoms of polycystic ovaries and many women without PCOS can have polycystic ovaries. Your ovaries, after all, are cyst making machines that pump out cysts every month that mature into ovum and set out on their journey to meet their one true sperm. Polycystic ovaries can only be diagnosed with ultrasound and must meet a set measure to meet qualification for diagnosis. If a woman has any two of the three criteria, hyperandrogenism, menstrual irregularities, or polycystic ovaries, they meet criteria for a diagnosis of PCOS.
So what’s the big deal about having PCOS? Well remember that snowball effect I mentioned, this is what that comes to play. PCOS is like making a small snowball and pushing down a snow covered hill. It may start off small and innocuous but it can grow into a really big problem. PCOS is a hormonal disorder at its core. An increase in male hormones and unbound estrogen is what leads to the menstrual disturbances. These hormonal irregularities cause anovulation. Meaning those cysts that your ovary creates do not regularly turn into the ovum that can be fertilized. This is what leads to the increased menstrual cycle length or complete lack of menses. If there’s no ovum for potential fertilization,there’s no build up of endometrial tissue inside the uterus, preparing for the possibility of pregnancy, and there’s no shedding of that tissue when fertilization doesn’t occur. For these women, many women with PCOS experience infertility. You must ovulate in order to potentially become pregnant.
The hormone disturbances in PCOS also lead to insulin resistance. Obesity, a BMI greater than 30, is not a diagnostic criteris of PCOS but due to the insulin resistance associated with the disorder many women with PCOS are obese. However, you can also be normal weight and meet criteria for diagnosis. Studies have shown that even normal weight women with PCOS have some degree of insulin resistance. Insulin resistance causes your body to produce more insulin which in turn leads to the production of more male hormone and increased fat cell production.
The most important thing to note about PCOS are the medical sequelae that can occur. Women with PCOS have an increased risk of developing metabolic syndrome which is a grouping of conditions that increase your risk of cardiovascular disease and diabetes. These include obesity, elevated High density lipoprotein (HDL) and triglyceride levels, increased blood pressure and increased blood sugar levels. Up to 60% of young women with PCOS and a BMI greater than 30 can have metabolic syndrome. PCOS also increases your risk of diabetes by 2-5 times the normal rate due to the increased insulin resistance associated with the syndrome. Women with PCOS are also at a 2-3 increased risk of developing endometrial cancer due to the menstrual and hormonal irregularities that are hallmarks of the syndrome.
What can you do if you think you might have PCOS? The first thing to do would be to check in with your OB/GYN. PCOS must be diagnosed by a medical professional. PCOS can also be mistaken for other hormonal disorders and a full workup is warranted for diagnosis. There are treatments and lifestyle changes that can also help to minimize the effects of PCOS. Studies have shown that even a 5% weight loss for obese women with PCOS can lead to an improvement in symptoms. For women with PCOS who are not trying to conceive, oral contraceptives are also a great option to control symptoms of menstrual irregularity and are also proven to decrease the risk of developing endometrial cancer in the future. There are also effective treatments for infertility as well as male pattern hair growth that can be prescribed by your doctor.
PCOS is a complicated disorder and we are still unsure of why people develop the syndrome. But like in all things, knowledge is power. So instead of just attributing those irregular periods to stress or that upper lip hair to genetics I implore you to consider PCOS and to see your OB/GYN for a full evaluation. I encourage women everywhere to put your own health in forefront, because, well, YOLO.
Keemi Ereme MD, MPH
OB/GYN resident PGY2
References:
Lobo, R., Gershenson, D., & Lentz, G. (2016). Comprehensive gynecology (7th ed.). [Place of publication not identified]: Elsevier.
Polycystic Ovary Syndrome. (2018). Retrieved 24 May 2021, from https://www.acog.org/clinical/clinical-guidance/practice-bulletin/articles/2018/06/polycystic-ovary-syndrome